Research, new techniques improve results
By Martin Lenkowsky
Implanting devices in the brain to reduce the effects of Parkinson’s disease, making life-saving tourniquets available to average people, and educating students in the health sciences with lifelike mannequins are only a few of the featured stories in the latest installment of our series, “Innovations in Health Care.”
Stop the bleeding; save a life
If bystanders at the Marjory Stoneman Douglas High School shooting had been trained to stop bleeding, some lives might have been saved, says physician Igor Nichiporenko, trauma director at Broward Health North, where some victims were transported.
“Uncontrolled bleeding is the No. 1 cause of preventable death in a trauma,” Nichiporenko says.
An initiative called “Stop the Bleed” aims to educate the public on how to stanch blood loss, including by the use of tourniquets.
To help, Broward Health has purchased blood-loss kits and plans to make them available to the public. “A lot of cities will be rolling out programs to make them available,” says Kelly Keys, manager of Broward Health’s Emergency Preparedness Department. The kits, which include a tourniquet, a chest seal, QuickClot, and a pressure bandage, will be installed in large public access areas.
QuickClot also sells its products online.
A way to see your doctor
You wake up feeling lousy, but your primary care doctor doesn’t have an appointment until late next week.
Here’s a better scenario: you call Epic MD, a telehealth company. Within minutes you can speak to a doctor and get prescriptions sent to your pharmacy.
“Twenty-nine days is the average time for someone to get into a doctor’s office in the United States,” says Epic MD president Jack Karabees.
His company’s technology allows doctors to access patients’ medical history and communicate with them via phone, video and computer in a fashion compliant with federal privacy laws. Cost is $29 a month for unlimited consultations, or pay-per-use.
New detection method for prostate cancer
Boca Raton Regional Hospital’s Eugene M. & Christine E. Lynn Cancer Institute has a new method to biopsy suspected prostate tumors: fusing MRI images of the gland through a transrectal ultrasound. This provides a more-effective way to localize and determine clinically significant, high-grade tumors.
“Specific lesions of the prostate, especially very small ones, cannot always be captured by ultrasound due to its poor resolution,” says urologist David Taub. “Moreover, ultrasound targets the peripheral areas of the gland and can miss a material percentage of cancers located in the front, midline and top portions of it.”
But with the MRI/TRUS fusion technique, a patient with elevated prostate-specific antigen levels undergoes an MRI scan, which effectively reveals details in soft tissue. Radiologists review the scans and identify suspicious areas.
Later, in an outpatient procedure, an ultrasound probe examines the prostate, and software overlays the MRI images, which provides 3-D views of the gland. These fused images guide precise placement of biopsy needles.
“I liken the [use] of the technology to using a GPS to reach your destination, rather than going with an old-fashioned map,” Taub says.
Mapping an irregular heartbeat
Boca Raton Regional Hospital is the first in Florida, and only one of five centers nationwide, to noninvasively map irregular heartbeats in patients with chronic atrial fibrillation and other arrhythmias.
The Medtronic CardioInsight Noninvasive 3D Mapping System uses a 252-electrode sensor vest that is worn by the patient to match body surface electrical data with heart anatomy.
“The technology allows mapping of certain arrhythmias with high accuracy prior to entering the cath lab so that the entire procedure can be planned before touching the patient,” says physician Murray Rosenbaum, director of electrophysiology at the hospital’s Christine E. Lynn Heart & Vascular Institute.
This technology offers a chance to stop when no other treatment is effective, including cases where initial ablation has failed, he says.
PBG Medical Center first with new A-fib treatment
Palm Beach Gardens Medical Center is the first hospital in Florida to perform heart ablations with the HeartLight Endoscopic Ablation System. The visually guided laser balloon lets physicians see within the heart and, for the first time, pinpoint and treat the cause of atrial fibrillation at the source. So far, more than 4,000 patients with AFib have been successfully treated with the system.
“This therapy will have significant benefits for those suffering from A-fib,” says Dianne Goldenberg, CEO at Palm Beach Gardens Medical Center.” This technology will help those in our community who are dealing with this disease and allow them to have a more productive and active life.”
A new tool in the fight against heart disease
Holy Cross Hospital in Fort Lauderdale just added the Diamondback 360 Coronary Orbital Atherectomy System to combat coronary artery disease, which occurs when plaque accumulates on artery walls. Plaque can include calcium, which is the most difficult substance to remove, says interventional cardiologist Joshua Purow.
“This shaves off some of the calcium. It drills the calcium off the plaque. We can put a stent in with much better results,” he says. “The times we needed it, we have had a tremendous success rate.”
Some patients have been able to avoid bypass surgery.
New PAD treatment at Delray Medical Center
Delray Medical Center is the first U.S. hospital to perform robotic-assisted peripheral vascular intervention with the CorPath GRX System. The procedure—performed by physician Joseph Ricotta, medical director of vascular surgery and endovascular therapy for Tenet Healthcare—brings robotic assisted precision to percutaneous (needle puncture) coronary and vascular-intervention procedures.
“This technology and the availability of this procedure will have significant benefits for those suffering from peripheral artery disease,” Ricotta says.
PAD is a disease of blood vessels outside the heart that commonly affects arteries carrying blood to the legs.
“The fact that Delray Medical Center is the first hospital in the U.S. to perform robotic-assisted peripheral vascular disease interventions is just another reason why our cardiac and vascular program is such a jewel within our community,” says Delray Medical Center CEO Mark Bryan.
Surgery without cutting
Imagine going in for surgery, and the physician doesn’t need a knife. Sound futuristic? It’s already here.
Insightec uses incisionless, MRI-
guided, focused ultrasound to dissipate tissue or lesions without invasive surgery. The precise acoustic waves destroys only the intended tissue.
“A thousand of these waves converge on one point,” says Maurice R. Ferre, CEO and chairman of Insightec, a global company with an office in Miami.
Sperling Medical Group in Delray Beach uses it for neurological conditions, and University Health in Boca Raton uses it for women’s health.
The U.S. Food and Drug Administration has approved it for movement disorders, and it has been found to be effective against benign tremors.
An alternative way to treat seizures
For some patients with seizures, medication does not always work. However, doctors at Baptist Hospital in Miami have a new tool called a responsive neurostimulation device, which is implanted in the brain to reduce seizures.
“It senses abnormal activity in the brain, and sends out an electrical impulse,” says neurologist Alberto Pinzon. “It responds to what is happening in the brain. It recognizes electrical patterns in your brain.”
The small device is implanted in the skull, adjacent to the brain. It identifies unusual brain activity that can cause seizures, and, within milliseconds, sends out impulses to normalize brainwaves before a seizure can occur.
Pinzon says the 20 to 30 percent of patients with a seizure disorder not responsive to medication are candidates for the device.
Brain implants offer help for Parkinson’s patients
Deep brain stimulation, sometimes referred to as a brain pacemaker, can help bring relief to those afflicted with Parkinson’s disease, says Baptist Hospital neurosurgeon Justin M. Sporrer.
“Parkinson’s is a movement disorder where the ‘brain machinery’ stops working,” Sporrer says. “There’s a lack of dopamine, and your movement becomes rigid.”
Often, Parkinson’s patients are given medication to replace the dopamine, but that can lead to too much involuntary body movement.
Deep brain stimulation uses implanted electrodes to targeted areas in the brain that help control production of dopamine. During implantation, a patient remains awake.
It is not recommended for advanced stages of Parkinson’s, but Sporrer says DBS allows patients to have relatively stable dopamine levels and rely on less medication.
Bioidentical hormone therapy
Bioidentical hormones have their name for a good reason: They’re naturally occurring and are chemically identical to hormones produced in the human body, says Carolyn Zaumeyer, an advanced registered nurse practitioner. “They’re made from plant and animal products,” she says.
As we get older, our body’s hormone production declines leading to changes in how we think and feel. Decreased hormone production can lead to mental sluggishness, weight gain, loss of mental focus and energy.
Comparing bioidentical hormones to synthetic hormones is comparing “apples to oranges,” Zaumeyer says. “Synthetic hormones increase the risk of strokes and heart attacks. Bioidentical decreases the risk. It’s the exact same chemical as in the body.”
She says there’s little risk of negative side effects, because “you’re just giving the body back what it used to have.”
Artificial intelligence, machine learning good news for patients
Each year, 806,000 medical articles are published, says Steven G. Ullmann, director of the University of Miami’s Center for Health Sector Management and Policy.
“There’s no way for a doctor to keep up with that,” he says.
“That’s where artificial intelligence comes in. It can pick up new methodologies and very significant changes. When your doctor says, ‘Don’t worry; I’ve been doing this procedure for 30 years,’ that’s when you should worry. A doctor’s eyes are only so good at picking up stuff.”
Artificial intelligence is only an aid in diagnosis and treatment, Ullmann says. “AI uses data other doctors have observed and reported, and doctors can tailor-make not only a diagnosis but a treatment plan.”
He points to IBM’s Watson as an example of AI combined with machine learning.
“IBM Watson is able to take into account the 800,000-plus medical articles that come out every year,” Ullmann says. The IBM system can answer a physician’s questions and suggest diagnoses and current treatments.
A unique approach to an age-old problem
Men and women who suffer from hair loss don’t need to lose hope, too. Bauman Medical Hair Transplant & Hair Loss Treatment Center prides itself on using both comfortable and artistic restoration methods.
The company’s founder and CEO, Alan J. Bauman, is one of only a small number of physicians worldwide certified by the American Board of Hair Restoration Surgery. “I have always believed that one of my main responsibilities is to find the latest and most effective options that will help yield the best possible patient results, while also making their time with us as comfortable and enjoyable as possible,” he says.
Bauman says innovation is critical in his industry, citing his work pioneering minimally invasive, no-linear-scar follicular unit extraction hair transplantation harvesting in the late 1990s; robot-assisted hair transplants; and custom 3-D-printed prosthetic medical-grade hair replacement systems from Italy. Ultimately, however, he says, “it’s a people business, and providing the highest quality of service and patient care is paramount.”
Bauman offers video consultations for clients via smartphones, tablets or PCs. “This means that men and women looking for help with hair loss can start their hair restoration journey by having a private session with me, from the comfort and privacy of their own home,” he says.
Using sports as a motivating tool for the disabled
Sometimes, finding ways to motivate those with debilitating injuries or illness can be difficult. However, former professional football player Ray Shipman has found a way.
Shipman, who played linebacker for the NFL’s New Orleans Saints, is now director of the Adaptive Sports and Recreation Program for the Memorial Rehabilitation Institute, part of the Memorial Healthcare System.
The program uses recreational sports to inspire and motivate those who have been dealt some of life’s harshest blows—such as traumatic brain or spinal cord injuries, lost limbs, gunshot wounds and strokes.
Shipman starts by visiting patients in Memorial’s rehab department. “You build a rapport with them,” he says.
And what was his proudest accomplishment? “When our wheelchair basketball team finished No. 2 in the country. It took perseverance to keep competing at such a high level of competition.”
Learning facility feels like the real thing
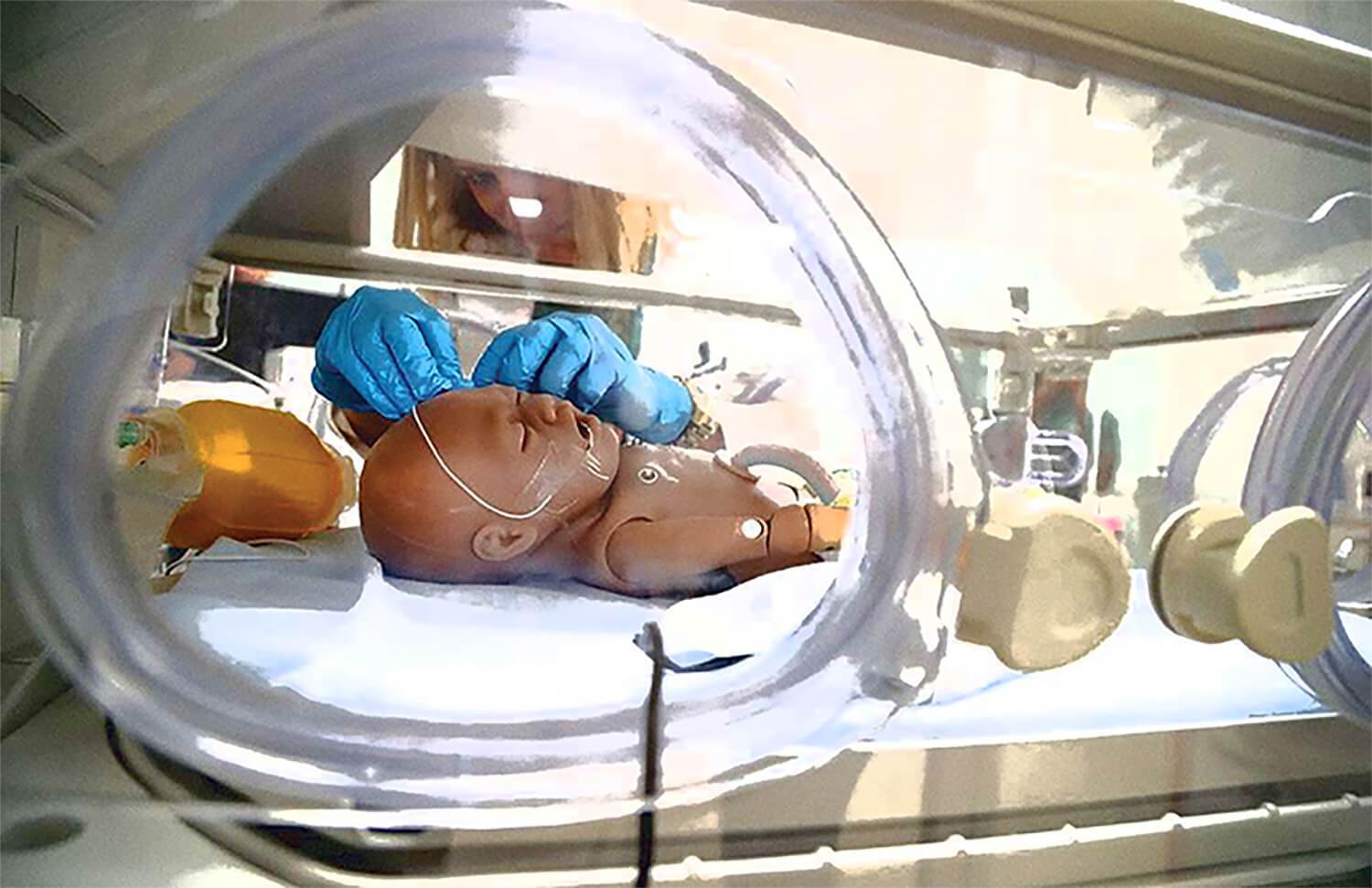
Students at the University of Miami’s School of Nursing and Health Studies can say they’re practically honing their patient skills at a hospital, because the school’s Simulation Hospital so closely mimics the real thing.
The five-story, 40,000-square-foot building is designed to have the look and feel of a complete, birth-to-death, full-service hospital, says Susana Barroso-Fernandez, assistant professor of clinical and simulation director.
The facility has a mock intensive care unit, delivery rooms and even an outpatient clinic. Students work on full-bodied mannequins with elaborate computer programs designed to mimic real patients. The mannequins can provide medical histories as well as exhibit symptoms of an impairment students have to diagnose and treat. “It’s an amazing teaching tool when done correctly,” Barroso-Fernandez says, adding that the facility will work with
fire-rescue agencies, other allied health professionals and the business community, which can rent space.
Corporate fitness provider arrives
Gympass, an international corporate fitness benefit provider, has opened in Miami as part of its U.S. launch.
Says Gympass co-founder and CEO Cesar Carvalho: “We are thrilled to bring Miami into our worldwide network of 5,000 cities in 13 countries and counting.”
Gympass partners with corporations to give employees an affordable gym membership with unlimited access to a global network of more than 30,000 fitness facilities in 13 countries.
Employees typically receive 50 to 70 percent off market prices, and the employer pays for 5 to 10 percent of the total subsidy.
Two large corporate partners in South Florida are slated to come on board later this year.
Cleveland Clinic Florida continues to spread its roots
Cleveland Clinic Florida has opened a new medical office in Wellington and plans to open a new Coral Springs facility in July.
The clinic’s 7,400-square-foot facility is in the Village Green Center, at the corner of Stribling Way and State Road 7. It will offer primary care, gastroenterology, cardiology and other specialty services with 22 examination rooms and physician offices.
“We are excited about opening our first location in western Palm Beach County, which will provide Cleveland Clinic Florida patients with expanded access to world-class care and greater convenience,” said physician Wael Barsoum, president of Cleveland Clinic Florida.
The 72,000-square-foot Family Health and Ambulatory Surgery Center at 5701 N. University Drive in Coral Springs will offer specialty care, outpatient surgical services and imaging services. The facility will include six operating rooms; 24 preparation and recovery bays; two endoscopy suites; CT/MRI, mammography and X-ray imaging services; and 40 exam rooms.
A 180,000-square-foot multi-level hospital tower will open in July at Cleveland Clinic Florida’s main campus in Weston. The new building is designed to accommodate surgical cases from medical specialty areas and Broward County’s largest transplant program.
The clinic also will add 75 more hospital beds; three operating suites; critical care areas; 25 percent more emergency room capacity; a new women’s center; a larger cafeteria; an expanded laboratory and imaging facilities; and more parking.
High-tech tattoo removal
Some mistakes can be erased, says Claudio Sorrentino, founder and CEO of Body Details, which specializes in laser removal of hair and unwanted tattoos.
As tattoos grow in popularity, so does regret as people decide their body art no longer means as much as it once did. Sorrentino says nearly two-thirds of people between ages 18 and 44 have ink.
In addition to removing tattoos, Body Details also removes unwanted hair and skin imperfections with a PicoWay laser, the strongest approved by the FDA. It also offers laser skin rejuvenation.
Based in Boca Raton, Body Details has seven South Florida locations and offers a lifetime guarantee on its services.
Body Details uses medical professionals—advanced nurse practitioners and physician assistants—to work with patients. All work is certified by a board-certified plastic surgeon. ♦