By Clarissa Buch and Sally-Ann O’Dowd • photography (where indicated) by Eduardo Schneider
“It’s so terrifying because as a pregnant female, I’m considered immuno-compromised. If I get infected, my immune system won’t be able to fight off the virus as well.”
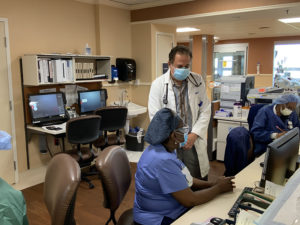
Edmara Nieves
Attending physician, emergency room,
Broward Health Medical Center

Background: Nieves earned her medical degree at Ponce Health Sciences University School of Medicine in Puerto Rico and completed her residency at Orlando Health. She teaches emergency medicine to students and residents as a faculty member at Nova Southeastern University and Florida International University.
Pandemic stories: Fear strikes the Broward Health Medical Center ER team when paramedics call from the ambulance to say they’re bringing in a COVID-19 patient in respiratory distress. “We don’t know if we are doing enough to protect ourselves,” Nieves says. “There’s a reason why [some 800] U.S. health care workers have died because of COVID [as of mid-July, according to reporting by The Guardian and Kaiser Health News].”
Pregnant with her first baby, a boy who is due in September, Nieves has been particularly worried about her health.
“It’s so terrifying because as a pregnant female, I’m considered immuno-compromised,” she says. “If I get infected, my immune system won’t be able to fight off the virus as well as if I weren’t pregnant.”
Her gynecologist suggested she stop working, but she didn’t want to abandon her team in a time of need. Although she did perform some “crash intubations” when the pandemic first hit—the insertion of a tube into a patient’s trachea—she no longer gets that close to sick patients; her team members do the procedure instead.
“It’s one of the scariest times in our professional career,” she says. “We go into medicine, and we spend over 10 years just studying to learn the diagnostics and therapeutics that have proven to be safe and efficacious. But now this pandemic comes in, and we’re facing this giant with little to no evidence about what works.”
She recognizes the emotional and financial burdens of the spring lockdown. But from a physical health perspective, Nieves saw its benefits.
“People were staying home, they were being good, so the COVID volume went down significantly” in May, she says. “We were feeling very hopeful.”
But a false sense of security led to what she calls “a 180-degree turn.” In July, more than 60% of the visits to Broward Health’s ER Room were COVID-19 patients, she says.
As South Florida makes headlines as a viral epicenter, Nieves reflects with chagrin on the community’s handling of the pandemic. People are resuming normal activity without wearing masks.
“It came to a point where we became comfortable with the situation, with the numbers we were seeing, with starting up our lives again,” she says. “We dismissed the highly virulent, life-threatening enemy. The virus is still here—it was just waiting for us to make a mistake.”
“The chest X-ray was probably the worst I’ve seen in four years. We ordered an ambulance right away and called her family. She was ultimately placed on a ventilator for weeks.”
Makandall Saint Eloi
Associate medical director, University of Miami/Jackson Memorial Hospital Urgent Care

Dr. Saint Eloi with his fiancée at an event celebrating his recognition as a “health care hero”

Background: Saint Eloi, 31, is a young leader in the medical field working diligently on the front line of the current pandemic. Before COVID-19, the Miami-based doctor served as chief resident of his medical class at the University of Miami and later joined the staff at Jackson Memorial Hospital, working in the ER and UHealth Jackson Urgent Care locations.
Pandemic stories: Saint Eloi remembers expressing initial concern about COVID-19 to his mother and brother in late 2019. By mid-February, he realized the pandemic would be the worst medical disaster of his career.
“It’s kind of ironic because when I was little, I always told my mother that I wanted to be the doctor who found a cure for HIV, AIDS or another type of virus,” he says. “That’s what motivated me to study medicine in the first place. But I never actually thought I would be working during a pandemic like this.”
Saint Eloi’s first coronavirus patient at Urgent Care was a woman in her late 50s, who presented with fatigue, shortness of breath, coughing and a lack of appetite. He immediately put an oxygen monitor on her finger and ordered a chest X-ray. Her results left him in shock.
“The chest X-ray was probably the worst I’ve seen in four years,” he says. “We ordered an ambulance right away and called her family. She was ultimately placed on a ventilator for weeks.”
Though the patient was sent home about a month later, she has a long road of recovery ahead of her, Saint Eloi says. “Everyone keeps talking about recovery, but recovery is very subjective,” he says. “It doesn’t mean you’re back to your baseline. All it says is you’re stable enough to go home. This patient in particular was discharged on oxygen and blood thinners. These factors have changed her quality of life, at least for the foreseeable future.”
In addition to treating patients at Urgent Care since the spread of COVID-19, Saint Eloi has been an advocate for appropriate testing and evaluated patients daily who received a positive diagnosis. He has organized several free medical checkups for underserved communities in South Florida, remaining tireless in providing community initiatives both at Jackson Health System and in his home country of Haiti.
“Even in this short period of time, people I’ve worked with, family members, and friends have all been affected by the virus,” he says. “It has become very personal. Though COVID-19 may not seem serious to everyone, there’s always someone outside—a grandparent, a mother, an infant—who may be detrimentally affected by this. Every life is important, and this goes far beyond more than just one person.”
“[restaurants] helped us raise $315,000 for [for a ja fundraising event] and now, two months later, their business capacities were limited,” Homan says, recalling the challenges facing the restaurant industry after the shutdown. “When you’re a charity, you’re on the receiving end a lot, and when you can stand up and give back, you do.”
Jennifer Homan
Vice president of development,
Junior Achievement of South Florida

Background: In her role at Junior Achievement, Homan raises funds to deliver financial literacy, workforce readiness and entrepreneurship programs to 52,000 students a year. The Aventura resident earned her bachelor’s degree in psychology from Michigan State University and a master’s degree in mental health counseling from Nova Southeastern University.
Pandemic stories: “When the COVID-19 pandemic hit, Junior Achievement didn’t miss a step, immediately transitioning to continue to meet the needs of teachers, students and parents by providing curriculum on digital platforms,” Homan says. “It was a fast-paced response effort to limit the disruption in education as much as possible.”
At the same time, the lockdown was putting severe financial strain on many of the restaurants that had supported the popular JA Uncorked fundraising event (last held in January). When her sister, a hospital administrator in Michigan, told her she barely had time to eat, Homan saw an opportunity to help both the local restaurant industry and essential workers.
“They helped us raise $315,000 for the event and now, two months later, their business capacities were limited,” Homan says, recalling the challenges facing the restaurant industry after the shutdown. “When you’re a charity, you’re on the receiving end a lot, and when you can stand up and give back, you do.”
She called the effort Medi-Meals, an effort she kickstarted in March with a $500 donation of her own. She designed a logo, created a GoFundMe page, and sent a link via Facebook to her network. By the next morning, she had collected more than $2,200.
Over the next five weeks, 80 donors contributed $8,200 to provide food for workers at Broward Health, Memorial Regional Hospital, UM Sylvester Comprehensive Cancer Center, Aventura Hospital and Holy Cross Hospital. Homan developed a budget to maximize the resources, paying the restaurants about $8 a meal. Casa Calabria in Fort Lauderdale, for example, provided spaghetti and meatballs, bread and a side salad; Quarterdeck restaurants made club sandwiches and sushi; Capital Grille made truffle macaroni and cheese.
In all, some 15 restaurants and culinary businesses received billable orders and/or donated food, including Hoffman’s Chocolate, It’Sugar, Village Tavern, Smokey Bones, Spatch Peri-Peri, Tap 42, and Firehouse Subs. Homan and her son, Jakyb, 18, made nightly deliveries, dropping the food off at the curb of ER entrances. Hospital staff would pick it up and wheel it inside on a cart.
For mother and son, Medi-Meals is a sign that people are fundamentally good. “It was a very dark time,” Homan says. “The first [instinct] was to help. Everyone came together.”
“Seeing how bad this can turn and what coronavirus can transform into … it changes you. Protect yourself. Protect others. If you must leave your house, be smart about it. Wear a mask.”
Anakarla Perozo
Trauma ICU nurse, Kendall Regional Medical Center

Background: As the first member of her family to pursue a career in medicine, Perozo, 29, has had a desire to help people for as long as she can remember. “My mom always wondered why I wanted to do this,” she says. “There [are] no doctors in our family. It came out of nowhere.” After moving to Miami from Cuba more than a decade ago, Perozo enrolled in Miami-Dade College and then Florida International University to study nursing. She began her career at Westchester General Hospital and later transitioned to Kendall Regional, a Level 1 trauma center, to work in the ICU. This August marks one year working with some of the hospital’s sickest and most critical patients. “This is what I’m going to do my entire life—pandemic or no pandemic,” she says. “In the ICU, you have the chance to change a patient’s life forever.”
Pandemic stories: Two years ago, when Perozo began her career in nursing, she never imagined she would provide care to patients during a pandemic. Though medical professionals like Perozo prepare for this moment throughout their practice, many never experience an outbreak like COVID-19.
“COVID-19 is like going back to school,” she says. “We’re learning more every day to help our patients.”
The hardest lesson Perozo has learned is the need to protect herself before assisting others. It’s something she still struggles with today, months into the fight against coronavirus.
“Before COVID-19, I would see a patient in need and drop everything to help them,” she explains. “You forget about the precautions and protocols. Your first thought is to save their life. That’s still true today, but if I don’t protect myself, and I get infected, what help am I then?”
One of Perozo’s first experiences with the virus was a 55-year-old woman, the same age as Perozo’s mother, who was put into the ICU after her diagnosis. Though the woman wasn’t Perozo’s patient, she watched from a distance as doctors attempted to stabilize her.
“She was bleeding from everywhere you can think of,” Perozo remembers. “I’ll never forget when one of the doctors said they were going to have to warn the family that this would be the end, and they had done everything they could to try to save her.
“Seeing how bad this can turn and what coronavirus can transform into … it changes you. Protect yourself. Protect others. If you must leave your house, be smart about it. Wear a mask.”
Perozo is bracing herself for subsequent virus peaks, which she expects to see through the new year and possibly beyond. “This is really, really bad,” she says. “We go from the unit being empty and thinking we experienced the worst of it to, out of the blue, dozens and dozens of cases. This is our new normal.”
“There’s no way to know if … this will be the last time the patient speaks with their family. There’s also no way to know if … this is the last time a loved one sees their family member alive.”
Mauricio Danckers
Medical director,
Intensive Care Unit, Aventura
Hospital & Medical Center

Background: As medical director of the ICU, Danckers specializes in the care of the medical and surgical critically ill. In addition, he is an assistant professor of clinical medicine at Nova Southeastern University’s Kiran C. Patel College of Allopathic Medicine, where he was recently awarded Teacher of the Year for his commitment to graduate medical education. Board certified in internal, pulmonary and critical care medicine, Danckers is uniquely positioned to fight the coronavirus pandemic from all angles––both as a doctor treating patients on the front lines, and as a director helping ensure the hospital remains as prepared and equipped as possible.
Pandemic stories: Since the outbreak of COVID-19, Danckers has witnessed the sheer panic that overcomes patients just minutes before they are placed on ventilators due to COVID-19 complications.
“We’re up close and personal with the virus,” he says. “It hurts, and it’s incredibly challenging, both as a doctor and a human being.”
He has watched as they scramble to text and phone family members, with warnings that this may be their last phone call. “There’s no way to know if in these moments, this will be the last time the patient speaks with their family,” he says. “There’s also no way to know if in these moments, this is the last time a loved one sees their family member alive.”
Weeks before the pandemic reached South Florida, Danckers and his team of ICU medical professionals were busy preparing for the worst. No one could have predicted what they would ultimately experience. “April was a really harsh month,” he says. “We lost a lot of people, and we saved a lot of people. We thought that was the worst of it. Now we know we were wrong. This is our new reality.”
Similar to most medical professionals, Danckers never pictured himself fighting a pandemic. Though he has been in the field for more than a decade, the ramifications of COVID-19 are still difficult to grasp.
“Physicians are not supposed to be scared,” he says. “As an ICU doctor, I run into the problem, not away from it. We see the sickest of the sickest. … But health care professionals are human, too. We can get sick, we have families we’re worried about, and above all, we’re doing our best to treat every patient without overwhelming the system.
“Coronavirus has proven to be an uphill battle. This isn’t something that will come and go. This is reshaping the way we see the future.”
“It’s time to appreciate what matters, like a hug, holding hands, or even a smile. With coronavirus, we don’t even have that. … You can’t see a smile through a mask. … What I know for sure is I will never take these moments for granted again.”
Mireya Toquica
Nurse, Aventura Hospital & Medical Center

Background: Toquica, 34, was born in Colombia; she moved to Miami in 2000 with lifelong dreams of becoming a nurse. “I grew up in a place where people lacked basic health care resources and services,” she explains. “Seeing that changes you. That’s what inspired me to make a difference.” Shortly after settling in the United States, Toquica vowed to learn English, enroll in college, and dedicate herself to helping as many people as possible by pursuing a degree in nursing. She has worked at Aventura Hospital for the last three years as a medical and surgical nurse. Currently, she is stationed on one of the facility’s dedicated COVID-19 floors.
Pandemic stories: Similar to hospitals around the country, iPads have become the new handholding during the COVID-19 pandemic, Toquica says. These sleek, slender devices are lifelines for patients, especially for those receiving treatment on the COVID-19 floors.
“You truly can’t imagine how difficult it is for patients and families to not see each other and hold hands, especially during a pandemic,” Toquica explains. “This technology has become essential for us. It’s the only way patients and families can communicate.”
As a nurse, Toquica not only treats patients, but she also provides vital emotional support. As hospitals prohibit family and friends from visiting patients, she has found herself comforting patients in ways she never anticipated.
“I don’t know how we would do it without this technology,” she says. “Most patients, especially older ones, don’t come in with a mobile phone that has the capability to FaceTime. Patients being isolated from their loved ones is difficult enough.”
Nursing requires Toquica to live life a few steps ahead, anticipating what may come next and how best to prepare. However, working in the field during a pandemic has taught her the importance of slowing down and appreciating the small moments.
“We’re all in such a rush,” she says. “It’s time to appreciate what matters, like a hug, holding hands, or even a smile. With coronavirus, we don’t even have that right now. You can’t see a smile through a mask. Imagine talking to your loved ones for the last time through an iPad. What I know for sure is I will never take these moments for granted again.”
“A lot of the policies and protocols are constantly changing. It’s important to be transparent with the team. I don’t care how many times they ask me questions or call me. It’s my job to ensure that not only do they have the things to be safe, but that they know they are safe.”
Lina Puntervold
Nurse and infection control practitioner,
Joe DiMaggio Children’s Hospital

Background: Puntervold earned a master’s degree in public health with a minor in epidemiology from the University of South Florida. Having cared for the hospital’s tiniest patients in the neonatal unit, the Broward County resident now dedicates herself to disease-related research, reporting, and education.
Pandemic stories: Puntervold will never forget that March 7 was a Saturday. She was enjoying the weekend at home with her husband and their two children when she received a hospital alert. She was used to being on call; normally a phone discussion or email would satisfy the situation.
This time, she needed to drop what she was doing and report to work.
“I knew that [the need to go to the hospital] meant something else was going on, and my gut said it was related to COVID-19,” Puntervold says. “A few of us had been meeting to discuss strategic planning for Memorial Healthcare System’s six hospitals and how best to approach what was coming down the pike. I thought, ‘This is really happening.’”
JDCH treated 22 pediatric patients with COVID-19 through the first week of July. Through it all, Puntervold’s role has been the creation of protocols ensuring the safety of the people inside the 226-bed hospital, which treats children and adolescents suffering from illnesses ranging from leukemia to heart defects. The hospital has seven operating rooms and an entire floor dedicated to pediatric oncology. Given the presence of newborns and cancer patients—and their weakened immune systems—safety measures must be beyond reproach.
One of the hardest decisions was to set limits on who could visit the sick. As the world’s only children’s hospital to earn the Certification for Excellence in Person-Centered Care from the nonprofit health care consultancy Planetree International, Joe DiMaggio views the presence of a patient’s family and loved ones as essential to the healing process. Usually, there are no visitor restrictions.
“But because of COVID-19, we had a change in policy. We had to make the difficult decision of restricting visits to parents,” she says. “Unlike our sister hospitals, we weren’t going to close our doors to parents.”
At the same time, Puntervold has led communication efforts to educate employees about safety precautions, relying on guidelines from the Centers for Disease Control and Prevention. Since March, CDC recommendations have evolved; Puntervold remembers when masks and eyewear were not universally required.
“A lot of the policies and protocols are constantly moving and changing,” she says. “It’s important to be transparent with the team. I don’t care how many times they ask me questions or call me. It’s my job to ensure that not only do they have the things to be safe, but that they know they are safe.”
“We’re still in the first quarter of the phase of herd immunity. It could take up two years for natural herd immunity to develop; it would be much quicker with a vaccine.”
Melvin Kohan
Medical director, Infection Prevention and Control Program,
Broward Health Coral Springs
Background: The Wellington resident attended Universidad Autonoma de Guadalajara in Mexico, completed his residency in internal medicine at Mount Sinai Hospital at the University of Connecticut, and did his fellowship in infectious diseases at the University of Miami. Earlier in his career, he was acting director for the HIV and STD program at Broward County’s Department of Health.
Pandemic stories: “The pandemic will end,” Kohan says. “It will end.”
His perspective reflects history, personal experience and science. Kohan recalls the 1980s, when he worked with patients suffering from HIV before that disease even had a name. Back then, HIV was a death sentence. He was working at a Fort Lauderdale HIV clinic when AZT, the first drug that could fight the virus, received FDA approval.
Today, Kohan again finds himself treating people for a viral disease without a cure or vaccine. An absence of data “brings a lot of anxiety to us as physicians,” he says. “We’re learning as we go along.”
The memory of one man, in particular, stays with him. He was middle-aged and healthy before contracting the coronavirus in April. He came to the emergency room with a fever, low oxygen level and a dry cough. “He said, ‘Hopefully, I don’t get pneumonia,’ but unfortunately he did,” Kohan recalls.
Kohan, who teams up with a pulmonary specialist and intensive care doctor when treating COVID-19 patients, gave the patient numerous medications to treat the virus and secondary bacterial infections. They put him on a ventilator; he lay on his abdomen, unconscious, while blood clots formed in his body.
“He was beginning to wake up and seemed to be doing a little better,” he says. “Unfortunately, he died of a heart attack.”
Just as people with HIV can lead healthy lives, so, too, will society overcome COVID-19, he says. It will require herd immunity, which can take place naturally or via a vaccine. The virus could also mutate to a less virulent form.
With natural herd immunity, 70% to 80% of the population gets exposed to the disease and develops antibodies. Most people who get the disease will be asymptomatic and be “perfectly fine,” about 2% will get very sick and end up in the intensive care unit, and 1% to 2% of those who get it will die, Kohan says.
“We’re still in the first quarter of the phase of herd immunity,” he says. “It could take up two years for natural herd immunity to develop; it would be much quicker with a vaccine.”
When the FDA eventually approves a vaccine for safety and efficacy, people should get one, he says, offering another dose of hope.
“Pandemics do burn out. No one can predict the date, but it will end.”
“Am I scared? Maybe, but the overwhelming need to intervene and help those around me trumps any feelings
of fear.”
Lauren Green
Volunteer

Background: Green, 34, is a marketing assistant for a mortgage lender in Miami. Since the outbreak of the coronavirus, Green has shopped for countless friends and family who are unable to go to stores themselves. Word spread fast and she began shopping for nurses and doctors who were working long hours and could not secure items—such as Lysol, disinfectant cleaners and other essential items. As the need grew, she organized a fundraiser to help distribute meals to local hospitals.
Pandemic stories: Though Green doesn’t work in medicine, many people close to her––including family and friends––are doctors and nurses. Some are even immunocompromised. When she began to witness their fear over the COVID-19 pandemic, Green knew she had to find a way to act fast.
“None of them wanted to go inside stores,” she says. “I was scared too, but I figured the least I could do was offer to shop for their groceries and supplies and deliver it to their homes early in the mornings before working my full-time job.”
Since the pandemic took flight in Miami, Green and her husband have woken up before dawn almost daily, rushing to the nearest Walmart followed by Target and Walgreens before delivering as many supplies as possible to loved ones and friends.
“My friends have always called me ‘FEMA,’” Green says, laughing. “When I see an emergency or someone in need, even someone I don’t know, I try to help as much as possible. It could be me one day who needs the help, so I always try to go above and beyond.”
After weeks of shopping, some of Green’s friends in the hospitality industry suggested she organize free meals using leftover food that would otherwise spoil. So far, she has helped deliver meals to West Kendall Baptist and Nicklaus Children’s Hospital, with plans to tackle additional hospitals.
“As the cases start to rise again, I know our work is far from over,” she explains. “It’s incredibly rewarding to me. Every delivery I make, no matter how many times I’ve delivered to a friend or family in the past, I cry almost every time. Am I scared? Maybe, but the overwhelming need to intervene and help those around me trumps any feelings of fear.”
—C.B.







